Ndubuisi Akpuh1*, IkeOluwapo Ajayi2, Ayo Adebowale2, Hadejia Idris Suleiman3, Patrick Nguku1, Mahmood Dalhat1 and Elizabeth Adedire1
* Correspondence: drakpuh@gmail.com
Nigeria Field Epidemiology and Laboratory Training Program (NFELTP), 50 Haile Selassie Street, Asokoro, Abuja, Nigeria
Abstract
Background: Rivers State is among the states with high HIV prevalence in Nigeria. Occupational exposure to HIV through blood or body fluids of HIV/AIDS patients is a recognised risk factor of HIV infections among healthcare workers. We identified the determinants of occupational exposures to HIV among healthcare workers in Prevention of Maternal to Child Transmission (PMTCT) sites within Port Harcourt metropolis in Rivers State.
Methods: A descriptive cross-sectional study was conducted and a multi-stage sampling technique was used to select 341 healthcare providers from 22 public and 22 private health facilities in PMTCT sites in Port Harcourt metropolis. The data collected were analysed using descriptive statistics, Chi-square and logistic regression models (p-value = 0.05).
Results: Respondents’ mean age was 35.9 ± SD8.4 years, 270 (80.1%) and 171(50.7%) were females, and from public health facilities respectively. Prevalence of occupational exposure of healthcare workers to HIV in the past 12 months was 153 (45.0%), and 96 (63.3%) experienced such exposure more than once. Contacts with potentially infectious body fluid accounted for the largest proportion of 51 (33.3%); followed by needle stick prick 49 (32.6%). About 189 (56.1%) had safety information at their disposal and this serves as a reminder on safety precautions. The likelihood of occupational exposure was significantly higher among doctors (AOR = 2.22, 95% C.I = 1.16–4.25,) but lower among environmental health workers (AOR = 0.10, 95% C.I = 0.02–0.46,) than nurses/midwives when other factors were included in the model.
Conclusion: Occupational exposure to blood and body fluids remains a frequent occurrence among healthcare workers; highest among doctors in PMTCT sites in the study area. Provision of protective safety materials, training and enforcement of adherence to universal precaution strategies are highly recommended.
Keywords: Occupational exposure, HIV, HealthCare workers, Private facility, Public facility, PMTCT, Port Harcourt, Rivers State, Nigeria
Background
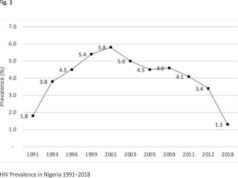
Human Immunodeficiency Syndrome (HIV/AIDS) is one of the infectious diseases that threaten human survival 1. Nigeria has the second-largest number of people living with HIV/AIDS (PLHA) in Africa accounting for 9.0% of the global burden with a prevalence of 3.2%, and burden of 3.1 million people living with HIV. This burden impacts negatively on the health system 2. Report of HIV research in Nigeria showed that Rivers State has the highest HIV prevalence (15.2%) among the states in the country (National AIDS Reproductive Health survey, 2014) 3, but the latest National HIV/AIDS indicator survey places her in the third position in prevalence amongst 36 states and Federal Capital Territory (Federal Ministry of Health, 2019) 4. Healthcare workers are exposed to infection-causing organisms, including HIV as a result of caring for patients in the health care settings and this often places them at risk of infection 5.
Healthcare workers have become infected with HIV in caring for HIV patients 5 through accidental exposure to body fluids and percutaneous injury (needle stick or cut with a sharp object), contact of the mucous membrane, or contact of skin (especially when the exposed skin is chapped, abridged, or afflicted with dermatitis 5–8. Unfortunately, unavailability of protective equipment and or healthcare workers’ refusal to use ‘the safety equipment where available increases the risk of occupational exposure 9.
This study focuses on how health care workers are at higher risk of occupational infection compared to other healthcare workers in non-HIV specialised facilities 10. It also focuses on specialized HIV care centres such as Prevention of Maternal to Child Transmission of HIV (PMTCT) sites in public and private settings 11. This is because PMTCT sites are designated sites for HIV patients, and the care they receive during labour and child delivery almost certainly entail revealing body fluids which can infect a health worker 12. There is a paucity of information on occupational exposure in private health care settings, and in HIV designated care centres in the available literature.
The objective of this study is to determine the prevalence of occupational exposure to HIV infection among healthcare workers in PMTCT sites and the outcome will make for policy direction from an informed perspective.
Methods
Study sites
Port Harcourt metropolis in Rivers State has designated PMTCT health facilities of public and private ownership. Private and public health facilities offer comprehensive healthcare services to clients. All study sites are reputed for a good volume of client turn out and had at least a representative of the healthcare worker of interest whose day to day activity requires their contact with an HIV patient or their body fluid.
An Interviewer Administered Questionnaire was used to assess the occupational exposure to HIV by asking about accidental splashes with the patient’s body fluids or prick by sharps while carrying out their duty. Also, their risk perception to occupational exposure, the practice of standard precaution procedure as well as the use of personal protective equipment. The availability of safety protocol/ regulation and method of waste disposal were also assessed.
Study design
We conducted a cross-sectional health facility-based study.
Study population
The study population was made up of healthcare workers such as doctors, nurses, laboratory scientists or technicians and environmental workers whose daily activities require caring for HIV infected patients.
Inclusion criteria
Healthcare workers in the selected health facility who were included in this study are doctors, nurses and midwives, laboratory scientist or technicians and environmental workers who were on duty and present at the time of visit; and gave their consent.
Exclusion criteria
Trainee healthcare workers, healthcare workers that had assumed administrative responsibility and those who are less than 6 months into posting at the present workplace were excluded from the study.
Sample size calculation
The sample size of 341 was calculated using the formula,
n = Z2 α pq
d2
Where,
n = the minimum sample size.
Zα = the standard normal deviate corresponding to level of significance of 5% = 1.96.
d = the desired level of precision, 0.05.
p = proportion of HCW exposed to needle stick injury in Northern Uganda = 0.28 13
q = 1- p = 0.72.
10% non-response rate brings n = 341.
Sampling technique
Multiple stage sampling technique was used to select the study subjects.
Stage 1: Health Facility Selection: All 22 public facilities within the study area designated PMTCT sites were sampled and an additional 22 of identified 34 private health facilities were selected by simple random sampling.
Stage2: Selection of health care workers from Health Facility: The study sample size of 341 was divided equally among the 44 selected health facilities giving 6 participants per facility.
Stage 3: Selection of cadre participants: At the facility, one health care worker was selected by balloting to represent each cadre of health workers among doctors, nurses/midwives, laboratory scientist or technicians and environmental workers. The remaining two health workers were selected randomly from the four cadres of healthcare workers in the facility. Where a facility had six health care workers, all were studied and where less the remaining is made up from another facility.
Pre-testing of data collection tool
Pre-testing of the questionnaire was conducted on 30 healthcare workers working in five health institutions that were not selected for the study before the actual data collection. Modification of logical sequence, simplicity, and clarity of the questionnaire was done using the findings at the pre-test.
Data collection
Data was collected using a semi-structured Interviewer administered Questionnaire. The questionnaire had three sections. Section A: socio-demographic characteristics of health care workers such as age, sex and occupation. Section B: Occupational risk exposure to HIV, and Section C: Determinant factors to occupational risk exposure to HIV infection. The questionnaire was partly developed by us and some variables adapted from previous similar published works 1.
Statistical analysis
We used Epi info 7 and SPSS statistical software to analyse descriptive variables and logistic regression to identify the independent risk factors associated with occupational exposure to HIV among healthcare workers using a p-value of < 0.05 as the level of significance.
Results
Of the 337 health care providers interviewed, 171 (50.7%) were recruited from public health facilities while. Sixty-three (18.7%) respondents were doctors, 124 (36.8%) nurses, 52 (15.4%) laboratory scientists or technicians, and 98 (29.1%) were environmental health workers. Study participants were predominantly Christians (336, 99.7%).
The majority (243, 72.1%) of the respondents had completed tertiary education. One-third (125, 37.1%) had worked for 10 years or more, and 246 (73%) work for an average of 40 h or more. Seventy-eight (23.1%) of the respondents were between the ages of 20–29 years, 156 (46.3%) were between the ages of 30–39 years, 75 (22.3%) were between the ages of 40–49 years, 24 (7.1%) were between the ages of 50–59 years and 4(1.2%) were 60 years old and above. The mean age was 35.9 ± 8.4 years in Table 1.
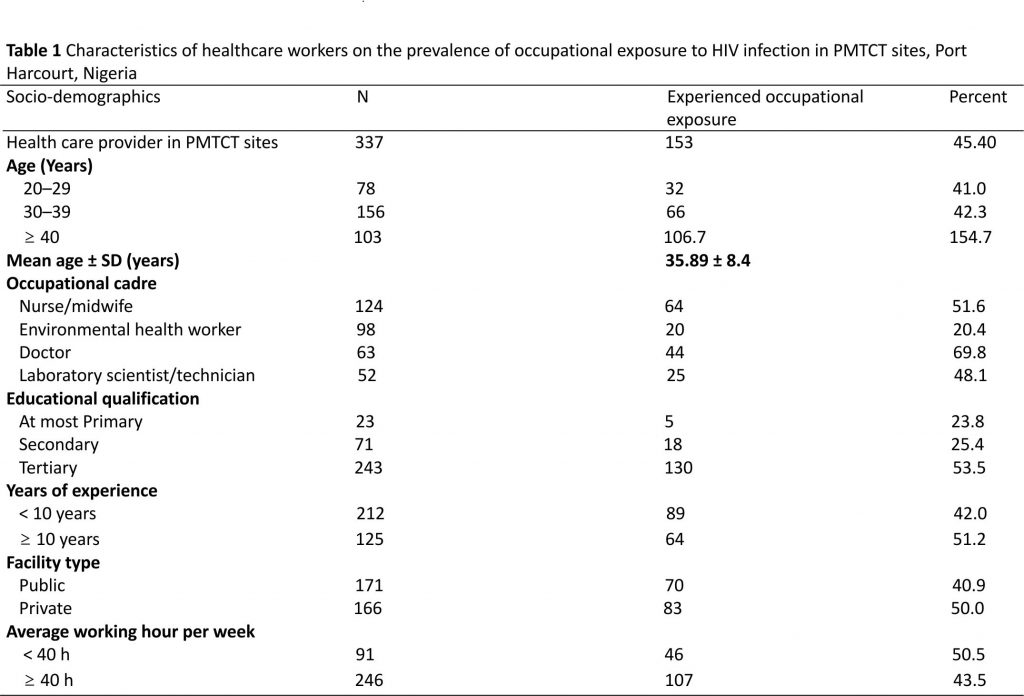
The data also depicts that the overall prevalence of occupational exposure to HIV infection among the studied health care providers in PMTCT sites in Rivers State was 45.4% (Table 2). Among health care workers in the public health facilities, the prevalence of occupational exposure to HIV infection was 40.9% compared to 50% reported by those who work in private health facilities.
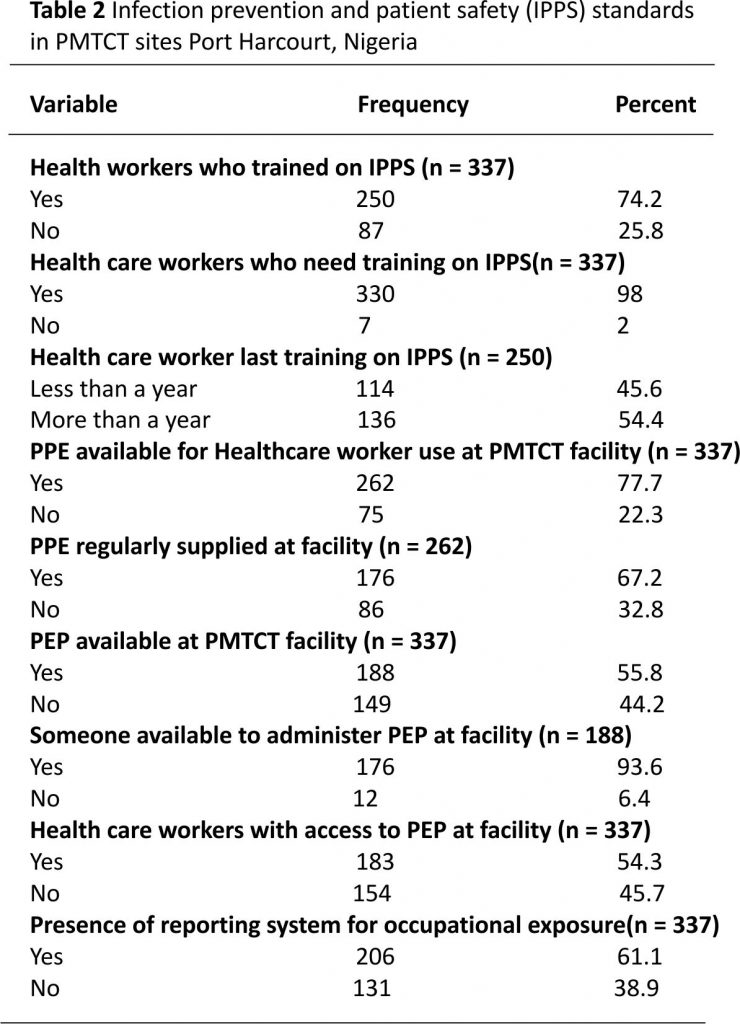 The prevalence of occupational exposure to HIV was as high as 69.8% among doctors and as low as 20.4% among environmental health workers. Higher prevalence was found among males (53.7%) than females (43.3%).
The prevalence of occupational exposure to HIV was as high as 69.8% among doctors and as low as 20.4% among environmental health workers. Higher prevalence was found among males (53.7%) than females (43.3%).
The prevalence increased with the level of education from 23.8% among those with, at most, secondary education to 53.5% among those with higher education. It was lower among those with less than 10 years working experience 89 (42%) compared to those with at least 10 years 64 (51.2%). In terms of the number of working hours in a week, the prevalence of occupational exposure was higher for health care workers who worked less than 40 h (50.5%) compared to those who worked 40 h or more (43.5%) in a week.
Age-specific prevalence revealed 15.7% among healthcare workers aged 40 years and 42.3% for those between the ages of 30–39 years then 41.0% for those between the ages of 20–29 years.
Less than half of the health care workers, 123(36.5%) always wear hand gloves in the course of their duty, while 185(54.9) wear hand gloves sometimes and 29(8.6%) never wear hand gloves (Fig. 1).
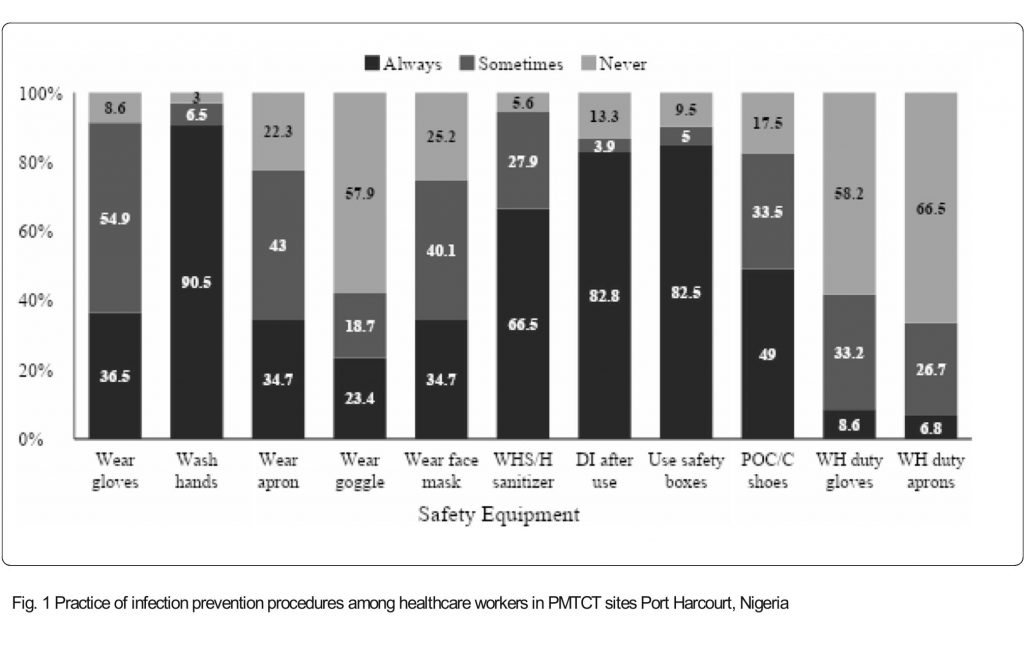
Almost all 305 (90.5%) of the healthcare workers wash their hands all the time, 22(6.5%) sometimes, and 10(3.0%) never wash hands while on duty. Regarding wiping hands with antiseptics, 224(66.5%) does it always while 94(27.9%) sometimes and 19(5.6) never. The face mask was always worn by 117(34.7%) and 85(25.2%) never did.
Up to 45(13.3%) of the respondents never decontaminated instruments immediately after use, 279(82.8%) always do, while 13(3.9) do some of the times.
A total of 278(82.5) respondents used safety boxes in the disposal of health waste, always as against 32(9.5) who never used a safety box. Regarding wearing personal protective equipment, only 168 (49.0%) wear protective shoes, 29(8.6%) use heavy-duty gloves, and much less 23 (6.8%) wear aprons while at work.
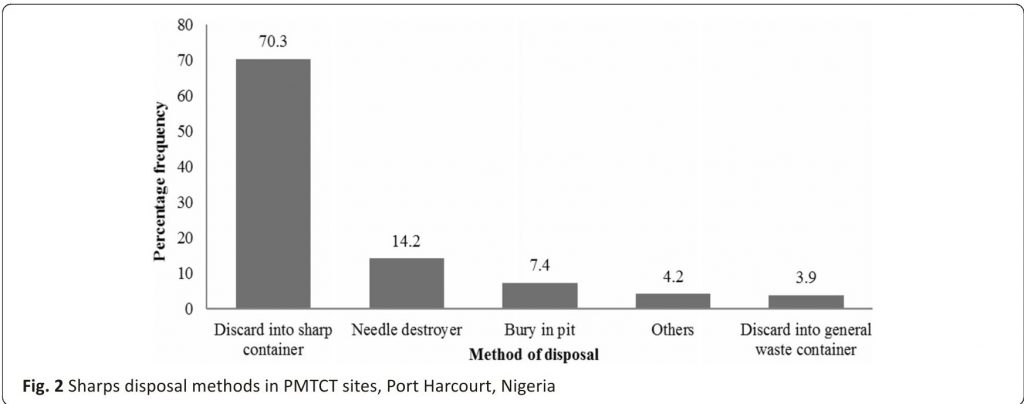
Figure 2 illustrates the disposal of sharps. Among the study participants, 237(70.3%) of respondents disposed of sharp equipment into containers set aside for sharps disposal. For some sharps like needles, 48 (14.2%) participants destroyed used needles in a needle destroyer, 25(7.4%) bury them in a health facility pit and 3.9% discard them into general waste containers. Only 4.2% dispose of sharps by other means that were not mentioned.
The main predictors of occupational exposure to HIV were career cadre. Doctors were more likely to have occupational exposure to HIV than another worker (AOR = 2.2, 95% C.I = 1.2–4.3, p < 0.05). On the other hand, environmental health workers appear to be protected when compared to nurses and midwives (AOR = 0.10, 95% C. I = 0.02–0.46, p < 0.01). Finally, there was no difference in risk of occupational exposure to HIV between health workers who work less than 40 h a week and those who work for at least 40 h (0.71(C. I = 0.44–1.12, p > 0.05) Table 3.
Discussion
Our findings indicate that about half of the healthcare workers had been exposed to HIV infection at their duty posts at one time or another in the past year prior to this study. These findings are consistent and similar to the Bosnia/Herzegovinian, Cameroonian, Saudi Arabian studies on the risk of occupational exposure conducted 11, 14,15. On the contrary, higher prevalence of occupational exposure to HIV infection among health care workers than the prevalence found in the current study has been reported by several other researchers in sub-Saharan Africa and other parts of the world 16. But, our findings on the prevalence of occupational exposure are above that obtained from similar studies conducted in Poland 10, Kuwait 17, South Korea 18 and Northern Nigeria 2. This difference in the prevalence of HIV observed in previous studies and our present study could be as a result of the difference in the study setting, study design and other methodological techniques. The differential in the level of training received by the health care workers in different study settings could also contribute to the variation.
It was also found that the prevalence of occupational exposure to HIV infection was higher among health care workers in private owned health facilities than their counterparts in the public health facilities; the same finding was observed in a similar study conducted in Cameroon in 2018 11. Higher prevalence observed among health care workers in private health facilities might be due to the fact that private health facilities are profit-oriented. Private health facilities are likely to function with reduced manpower and possible extended work hours per week in order to maximize profit especially in the phase of prevailing economic challenges in Nigeria. In the phase of present economic realities, the private health care facilities may not be living up to the expectations of ensuring their healthcare workers’ adherence to standard health and safety regulations in terms of providing protective tools and training on standard infection prevention techniques. On the other hand, the public health facilities attract support from donor agencies which include procurement of safety tools for healthcare workers as well as periodic training. This support may not be readily available at the private facilities because of the more corporate profile and patient selective nature of private health facilities compared to public health facilities.
The risk of transmission of HIV infection from patient to healthcare worker has been shown by previous studies to be 0.3% in percutaneous exposure and 0.09% in mucocutaneous exposure 19. Contact with the potentially infectious body fluid in both private and public facilities was found to be the commonest route of exposure to HIV infection in this study and it represents a substantive means of HIV transmission to a healthcare worker 20. However, this finding is different from other studies where sharp injuries were found to be the commonest 15. This outcome may be due to the fact that activities relating to dealing with sharps are more common among healthcare workers compared to dealing with activities that may cause splashes from body fluids. Other important risk factors to occupational exposures which were also found in this study and that could influence the experience of healthcare workers occupational exposure to HIV infection is lack of training on infection prevention and patient safety, unavailability and/ or irregular supply of personal protective equipment, and inadequate post-exposure prophylaxis and shortages of personnel to administer post-exposure prophylaxis. The existence of poor infection prevention modalities exposes healthcare workers to HIV infection in PMTCT setting 21. PMTCT sites at all times ought to function with the highest levels of infection prevention and control, given their nature as a specialized site where healthcare workers care for confirmed HIV positive patients and are at higher risk of contracting HIV compared to health workers in other non-HIV special-care health facilities either private or public.
In addition, we found that healthcare workers whose working hours were greater than 40 h were at higher risk of sustaining occupational exposure to HIV through percutaneous injuries and mucocutaneous contaminations compared with other healthcare workers is not unique as the similar study reported same in Mongolia 22. This is because fatigue and exhaustion could lead to lack of concentration and can further predispose the healthcare worker to occupational exposure.
Some of the facilities studied had no established system for reporting occupational exposures. This was similar to the situation reported in areas of comparable resource setting 23. The findings where a quarter of our study participants received no training on prevention of occupational exposure and almost all the participants wished to be trained on infection prevention and control is worrisome. These findings on deficient training on infection prevention are comparable to outcomes from similar studies in sub-Saharan Africa 21. The display of infection prevention and patient safety signs in health facilities is critical to the attitudes of healthcare workers towards infection prevention and patient safety practices. Our research indicates that about fifty per cent of the studied PMTCT sites had guidelines for infection prevention and patient safety readily on display. This situation is a common practice among health facilities in other similar studies in
The important predictors of occupational exposure found in this study were; a cadre of health care workers and length of working hours 26. Doctors were found to be at higher risk compared to other cadres of healthcare workers. This finding differs from findings from other studies where nurses were found to be at higher risk of occupational exposure 16, 27, 28. High risk found among doctors in this study could be attributed to the fact that they are particularly involved in carrying out invasive procedures, doing veno-puncture and repair of episiotomy.
Limitation of study
A potential limitation of the study includes self-report rather than records review which is a more reliable means of evaluation of occupational exposure as healthcare workers are bound to report socially accepted information. The ability to recall occupational exposure in the past is also a limitation. We adjusted for this by training interviewers and limiting the period of exposure within one year. Result interpretations and findings from this study may not be generalised beyond PMTCT sites because of the cross-sectional nature of study design.
Conclusion
The prevalence of occupational exposure to HIV infection among healthcare workers in PMTCT sites within Port Harcourt metropolis was high. Occupational exposure of health care workers to HIV infection is predicated upon the professional cadre of the health worker and high weekly working hours. In addition, the healthcare worker knowledge and adherence to the practice of infection prevention and patient safety are low. Also, despite the availability of protective equipment, all cadre of studied healthcare workers at one point attended to patients without protecting themselves. Some healthcare workers dispose of sharps instruments inappropriately. This implies that all health workers are at risk of HIV infection. Therefore, immediate training of healthcare workers on HIV infection prevention is recommended especially in privately owned PMTCT health facilities. There is also a need to enforce the display of infection prevention guidelines and protocol in the PMCTC sites within the constant reach and visualization of healthcare workers. All these are necessary to ensure the safety and protection of healthcare workers thereby making the fight against HIV transmission holistic.
Abbreviations
AIDS: Acquired Immune Deficiency Syndrome; AOR: Adjusted Odds Ratio; CI: Confidence Interval; HIV: Human Immune Virus; NFELTP: Nigeria Field Epidemiology and Laboratory Training Program; PLA: People Living with AIDS; PMTCT: Prevention of Maternal to Child Transmission of HIV; SD: Standard Deviation; SPSS: Special Package Statistical Software
Acknowledgements
The authors would like to appreciate Dr. Magbagbeola D. Dairo for his support and encouragement. We would especially acknowledge the NFELTP facilitators and host of others for their intellectual contributions towards the completion of this research. We are grateful to Dr. Mrs. Gloria Worugji for editing this paper.
Authors’ contributions
NA and AI made substantial contributions to the design of the study. NA was the principal investigator who designed data collection tools, collected data, analysed and interpreted data. AA assisted with data analysis and the draft of the manuscript. AI, AA, IS, MD, PN and EA revised article critically and made several important intellectual contributions. All authors’ have read and approved the manuscript.
Funding
No funding was secured for this study.
Availability of data and materials
The dataset used to produce this manuscript can be obtained from the corresponding author on reasonable request.
Ethics approval and consent to participate
We obtained ethical approval from the Scientific and Ethical Committee in the Department of Planning Research and Statistics of Rivers State Ministry of Health in a letter with reference number MH/PRS/391/Vol. 2/381. We obtained informed verbal consent from each participant as was approved by the ethical committee.
Consent for publication
Not applicable because data which could affect individual privacy was not indicated in the manuscript.
Competing interests
The authors declare no competing interest in connection with this paper.
Author Details
1Nigeria Field Epidemiology and Laboratory Training Program (NFELTP), 50 Haile Selassie Street, Asokoro, Abuja, Nigeria. 2Department of Epidemiology and Medical Statistics College of Medicine, University of Ibadan, Ibadan, Nigeria. 3Department of Community Medicine, Ahmadu Bello University Zaria, Kaduna State, Nigeria.
References
1. Tesfay FA, Habtewold TD. Assessment of prevalence and determinants of occupational exposure to HIV infection among healthcare Workers in Selected Health Institutions in Debre Berhan town, north Shoa zone, Amhara region. Ethiopia. 2014;2014: 2014.
2. Amoran OE. Occupational exposure, risk perception and access to prophylaxis for HIV/AIDS infection among health Care Workers in Northern Nigeria. Br J Med Med Res. 2013;3(2):275–87.
3. National Agency for the Control of AIDS (NACA), Federal Republic of Nigeria. Global AIDS Response Country Progress Report 2014. Available athttp://www.unaids.org/sites/ default/files/country/documents/NGA-narrativereport-2014 (accessed last 15 April, 2019).
4. Nigerian HIV/AIDS Indicator and Impact Survey (NAIIS) National Summary Sheet March 2019. Available at http://www.naca.gov.ng/naiis-nationalsummary-sheet/(accessed last 15 April 2019).
5. Gebresilassie A, Kumei A, Yemane D. Community Medicine & Health Education Standard Precautions Practice among Health Care Workers in Public Health Facilities of Mekelle Special Zone, Northern Ethiopia. J Community Med Health Educ. 2014;4(3):281.
6. Beyene T, Tadesse S. Predictors of occupational exposure to HIV infection among healthcare workers in southern Ethiopia. Int J Infectious Control. 2014; V10:i3.
7. Reda A A., Fisseha S, Mengistie B, Vandeweerd JM. Standard precautions: occupational exposure and behaviour of health care workers in Ethiopia. PLoS One 2010;5(12): 1–6.
8. Mashoto KO, Mubyazi GM, Mushi AK. Knowledge of occupational exposure to HIV: a cross-sectional study of healthcare workers in Tumbi and Dodoma Hospitals, Tanzania. BMC Health Serv Res. 2015;15(1):1–6.
9. Gumodoka B, Favot I, Berege ZA, Dolmans WM. Occupational exposure to the risk of HIV infection among health care workers in Mwanza region, United Republic of Tanzania. Bull World Health Organ. 1997; 75:133–40.
10. Garus-pakowska A. Behaviors and Attitudes of Polish Health Care Workers with Respect to the Hazards from Blood-Borne Pathogens: A Questionnaire-Based Study. 2019;1– 13.
11. Domkam IK, Sonela N, Kamgaing N, Takam PS, Gwom L, Michel T, et al. Prevalence and risk factors to HIV-infection amongst health care workers within public and private health facilities in Cameroon. 2018; 8688: 1–7.
12. Wu Q, Xue XF, Shah D, Zhao J, Hwang LY, Zhuang GH. Knowledge, attitude, and practices regarding occupational HIV exposure and protection among health Care Workers in China. J Int Assoc Provid AIDS Care. 2016;15(5): 363–9.
13. Odongkara BM, Mulongo G, Mwetwale C, Akasiima A, Muchunguzi HV, Mukasa S, et al. Prevalence of occupational exposure to HIV among health workers in Northern Uganda. Int J Risk Saf Med. 2012;24:103–13 Available from http://www.ncbi. nlm.nih.gov/pubmed/22751192.
14. Jahic R, Piljic D, Porobic-jahic H, Custović A. Epidemiological Characteristics of the Accidental Exposures to Blood-Borne Pathogens Among Workers in the Hospital. 2018;72(3):187–91.
15. Samargandy SA, Bukhari LM, Samargandy Shaza S, Bahlas RS, Aldigs EK, Alawi MM, et al. Epidemiology and clinical consequences of occupational exposure to blood and other body fluids in a university hospital in Saudi Arabia. Saudi Med J. 2016; 37(7): 783–90.
16. Gabr HM, El-Badry AS, Younis FE. Risk factors associated with needlestick injuries among health care workers in Menoufia governorate. Egypt Int J Occup Environ Med. 2018;9(2):63–8.
17. Omar AA, Abdo NM, Salama MF, Al-Mousa HH. Occupational injuries prone to infectious risks amongst healthcare personnel in Kuwait: a retrospective study. Med Princ Pract. 2015;24(2):123–8.
18. Lee JH, Cho J, Kim YJ, Im SH, Jang ES, Kim JW, et al. Occupational blood exposures in health care workers: incidence, characteristics, and transmission of bloodborne pathogens in South Korea. BMC Public Health. 2017;17(1):1–8.
19. Odongkara BM, Mulongo G, Mwetwale C, Akasiima A, Muchunguzi H V, Mukasa S, et al. Prevalence of occupational exposure to HIV among health workers in northern Uganda. Int J Risk Saf Med [Internet]. 2012;24: 103–13.
20. Wyżgowski P, Rosiek A, Grzela T, Leksowski K. Occupational HIV risk for health care workers: risk factor and the risk of infection in the course of professional activities. Ther Clin Risk Manag. 2016;12: 989–94.
21. Mossburg S, Agore A, Nkimbeng M, Commodore-Mensah Y. Occupational Hazards among Healthcare Workers in Africa: A Systematic Review. 2019; 85(1):1–13.
22. Markovic-Denic L, Maksimovic N, Marusic V, Vucicevic J, Ostric I, Djuric D. Occupational exposure to blood and body fluids among health-care workers in Serbia. Med Princ Pract. 2015;24(1):36–41.
23. Yi Y, Yuan S, Li Y, Mo D, Zeng L. Assessment of adherence behaviors for the self-reporting of occupational exposure to blood and body fluids among registered nurses: A cross-sectional study. PLoS One. 2018; 13(9): 1–13.
24. Jain M, Sabharwal ER, Srivastava D. Practices of health care personnel regarding occupational exposure. J Clin Diagnostic Res. 2016;10(11): DC 14–7.
25. Isah AM, Igboeli NU, Adibe MU, Ukwe CV. Evaluation of HIV post-exposure prophylaxis (PEP) in a tertiary health institution in South-Eastern Nigeria. J AIDS HIV Res. 2016;8(8):108–13.
26. Abdulmageed SS, Alabbassi F, Alradi M, Alghanaim N, Banjar S, Alnakhli M. Assessment of occupational exposure to sharp injuries among health care workers in king Abdulaziz University hospital. Int J Community Med Public Heal. 2018;5(5):1756– 61.
27. Motaarefi H, Mahmoudi H, Mohammadi E, Hasanpour-Dehkordi A. Factors associated with needlestick injuries in health care occupations: a systematic review. J Clin Diagnostic Res. 2016; 10(8):IE01–4.
28. Quan M, Wang X, Wu H, Yuan X, Lei D, Jiang Z, et al. Influencing factors on the use of standard precautions against occupational exposures to blood and body fluids among nurses in China. Int J Clin Exp Med. 2015; 8(12):22450–9.
Credits: Akpuh, N., Ajayi, I., Adebowale, A. et al. Occupational exposure to HIV among healthcare workers in PMTCT sites in Port Harcourt, Nigeria. BMC Public Health 20, 451 (2020). https://doi.org/ 10.1186/s12889-020-08528-5